My chronic Illness life has been a a bit hectic of late. Several changes. I was going to title this “New Stuff Coming Out of My Ears”, but thought readers might think I actually did have stuff coming out of my ears – I can assure I don’t. Not yet anyway!
I honestly didn’t quite know how to write about it all. I want to help other patients understand what may happen during their journeys and yet I wasn’t quite sure what was happening to me! So I kept quiet for a while until I could wrap my own head around the whole situation. Plus I wanted to be able to have a positive outcome to talk about. My main message to other patients is do not be afraid to ask the hard questions of your medical team if necessary. Some conditions/diseases are clear, others not so much. Medicine is not an exact science. My thyroid diagnosis was always clear: bloods and imagining are well established. Other conditions are not so easy to be accurate about, especially perhaps in the early days of the condition.
As some readers will know, earlier this year I moved to a different rheumatologist. We will call her Dr IV (Dr Four). I don’t exactly remember why now, but one of the things Dr IV did was send me for a brain MRI. That came back showing while the brain was actually pretty darn good, thank you very much, there is a small brain aneurysm. By small I mean somewhere between 4.5 and 5 mm, depending on who is measuring it, it seems. I am assured we don’t worry unless it is 7 mm. Now, to a doctor dealing with these things, 2.5 mm might seem like the size of the Grand Canyon. To the patient 2.5 mm is a pretty small difference! However, I’ll take the neurosurgeon’s word for it! The medical advice is to monitor. He did send me off for a CT scan as well, but at the time of writing I do not have the results – it was being done more as a baseline for future comparisons. This was, yes, a bit of a shock! (See update 1 below)
Around the same time I was referred by my previous sleep specialist to a colleague of his. Now this was interesting. His colleague, let’s call her Dr S2 (for Sleep Specialist Two), read my sleep study results from two years ago rather differently and recommended a CPAP machine. So this was a whole new adventure too. I will write about the CPAP experience in a later article.
After the above issues, and already on my THIRD PsA medication for the year, I asked both my GP and Dr IV, “Do we have the right diagnosis?”. My GP said, “Fair question!’. Dr IV kinda went “Hmmm” and wrote out a pathology request including tests I had not had for years.
Those tests came back as a bit of a shock! I have rheumatoid arthritis (RA) – the tests were pretty conclusive and my Rheumatoid Factor (RF) was, shall we just say, quite high. There was another test as well that when considered together with the RF is about as conclusive as you can get. My medication was changed that day. So medication number four for 2024.
By now my head was spinning a bit. Brain aneurysm, CPAP machine and a new arthritis diagnosis all in the space of a few weeks. Actually, it is an old diagnosis revisited, as I was first diagnosed with RA in 2014. Then in late 2018 that was changed to PsA. Now in 2024 I’m back to RA.
Or – do I actually have both? Dr IV and I are keeping an open mind on that question. Well, Dr IV more than me – after all she makes the call, not me! Let’s just say I would not be surprised to have both. It is considered rare, but not unknown.
Having both would also explain, I suspect, why I was getting worse – the PsA may have been being relatively well controlled, but in the background the RA was ramping up. I want to be VERY clear – that is MY thought at this time, it has not been suggested to me by my doctors, who are still investigating.
Since all of that, Dr IV has also ordered more blood tests, some of which are new to me. I do not know what the outcome of those will be, I had them done on Friday. (See update 2 below)
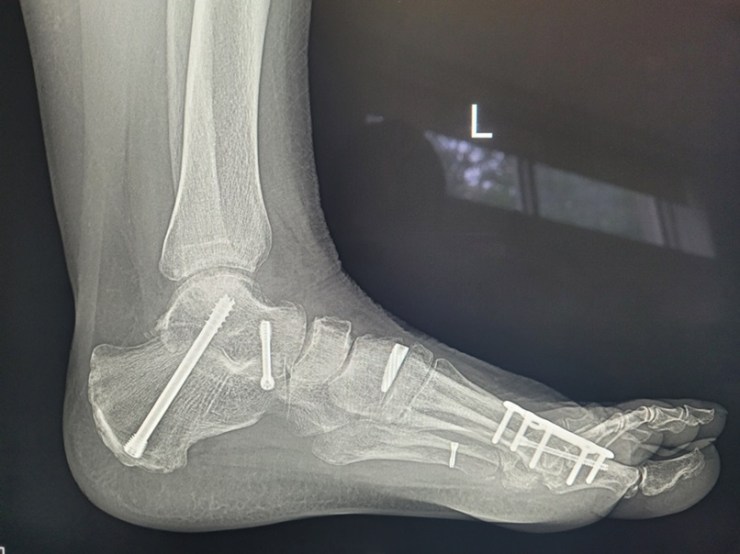
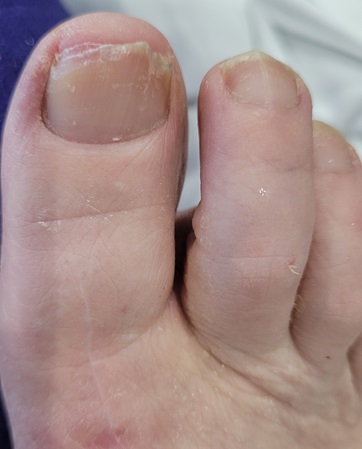
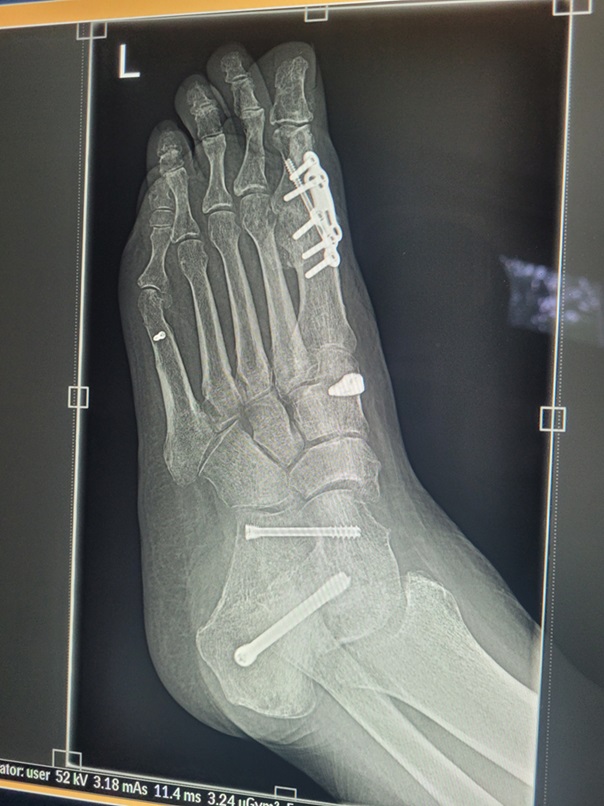
How did I feel during all of this? My emotions included anger, fear, relief, gratitude: each of which would come and go. Gratitude Dr IV was going all out to get to the bottom of the problem. Anger that the increase in RF hadn’t been picked up before, fear re the brain aneurysm before I knew the size, less fear (but a little) re the high RF which can be related to many things, not just arthritis. Relief there was an explanation for why I was so sore everywhere! At the time of the new/(additional) diagnosis, I had painful arm muscles, shoulders, wrists, elbows, neck, fingers. Even my wonderful replaced knees were sore. Worth noting when knees are replaced, the muscles, ligaments, tendons etc remain and they can still get inflamed by inflammatory conditions. It was comforting that during this time I coincidentally also had my twelve month final post-operative check with my knee surgeon and both knees looked perfect from a mechanical perspective on x-ray. So the knee pain had to be inflammation related.
As most of us know, some of these medications can take months to work. I was really surprised with my new medication this time. I’m not perfect yet (probably never will be), but I’m so much better than I was on the day I took the first injection! I am off Celebrex totally and only on 7.5 mg of prednisolone per day. Hope to get off that entirely, of course. My blood pressure has improved too (Celebrex may increase some people’s blood pressure and I may be one of those people).
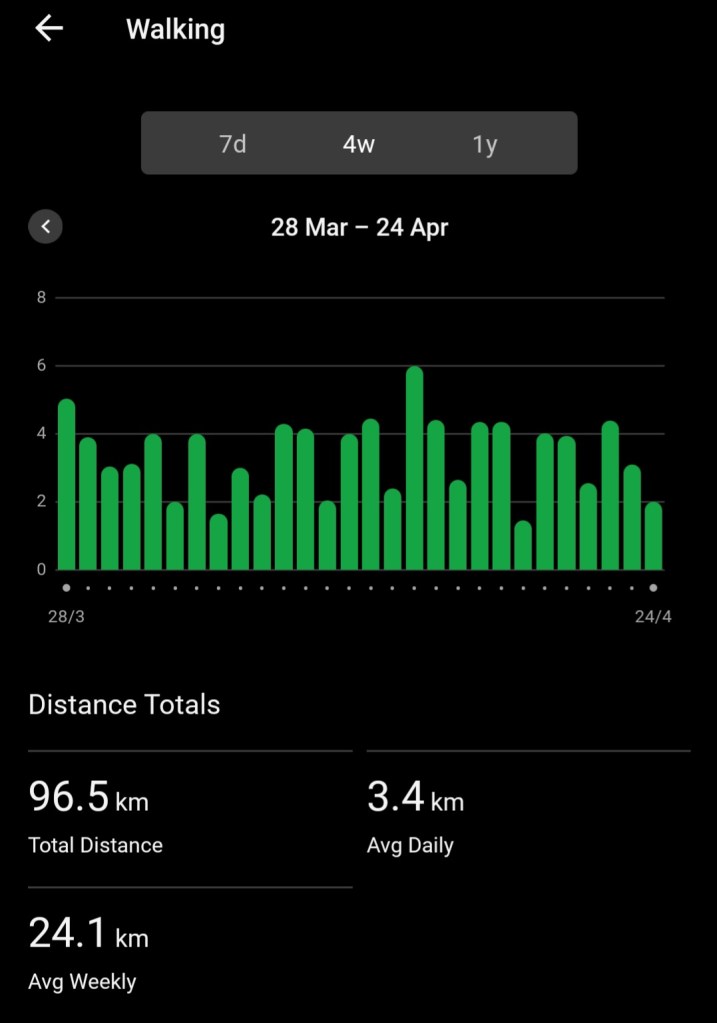
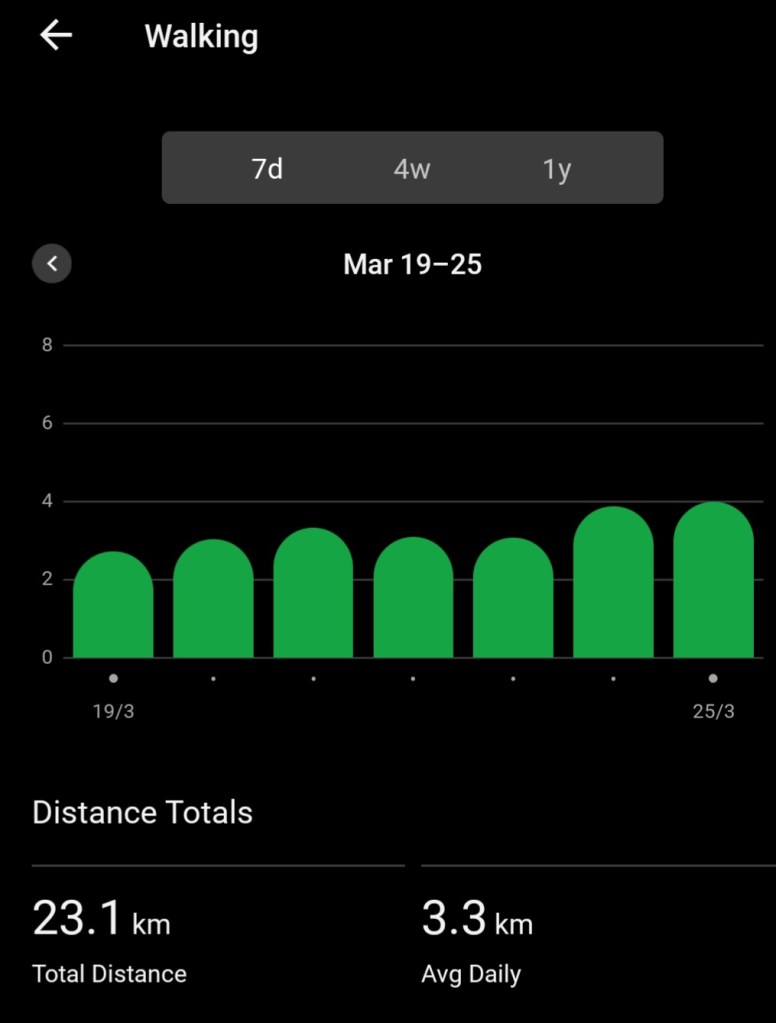
Today for the first time in ages I walked 3 km in one hit. I always walk 4 km a day, but lately 2 km has been my maximum distance in any single walk. Not only that, I did it at a pace of 11:51 minutes per km. I was very happy with that!

Thankfully, irrespective of whether I have RA, PsA or both, Movement As Medicine still applies. I don’t have to change my regime. In fact, Dr IV said to me she sees my dedication to Movement As Medicine as being what has got me through the years so far. That also made me happy.
This story isn’t over yet. There are more tests to come back, I still need to follow-up with the neurosurgeon for my own peace of mind and there is still the question of do I have both RA & PsA. The medication I am currently on treats both, which is comforting.
I have no sore bits anywhere. The capometacarpal joint areas of the index fingers are still both swollen, as are the areas around the ulnocarpal joints in both wrists. Dr IV tells me it can take a while for the swelling to go down. The heat of those swellings has gone. I am still limited with some finger mobility, but I’m working on the fingers and there are improvements. The top photo is my left hand today (can’t cross fingers), this photo is my right hand today (can cross fingers).

The video was captured last month. You can see on the left hand I can touch all my fingers to my thumb. On the right hand, not yet.
The best thing? No pain medications so I can hit the weights again (have done a few sessions already) and get those weights back up! Will I get back to 160 kg on the leg press? I don’t know, but I’m going to try!
Updates November 13, 2024
- I rang my neurosurgeon yesterday, just for peace of mind, for the CT results. That is when I discovered I forgot to tell his PA when I had the CT done. Where I had it done, they don’t send the results automatically. I burst into tears on the phone out of frustration at myself and embarrassment. The memory AGAIN. In fact, during that call, I could not even remember having the CT done, but I knew I had. I checked my calendar for the appointment and just after I found it, I REMEMBERED! It was in one of the rear buildings and I’d been trying to remember going to the main building. Nothing urgent about the results, but I will see neurosurgeon later this month to go through both the results and the plan for the future.
- I received a message yesterday that the blood tests done on Friday are not concerning, so THAT is a major relief!