Early in my chronic illness life, I wrote an introductory article, Pacing for Beginners. More recently, I wrote about Pacing THRU, Pacing UP, Pacing DOWN.
Pacing, balancing my life, has become even more critical since starting a full-time job. The earlier articles talk about the spoon theory and the battery analogy. Today I’m going to stick with the battery analogy as we all understand what happens when our mobile phone battery dies. That’s it. The screen is dead. You can’t make a call. The only option you have is to recharge the battery.
I find energy difficult to write about. I can’t quantify it like I can quantify calories or steps or weights. Energy seems elusive, hard to pin down. Even though I am using the battery analogy, I don’t have a charge meter on my arm. I can’t tell how much battery I have left at any given point in time. So if it seems like I’m pondering as I write, it is because I am pondering as I write.
Many of us with chronic conditions are a bit like a mobile phone. The battery has a limited capacity. I’ve written about fatigue/lethargy before too, in When was the Last Time You Yawned? Working full-time hours again, I have had to revisit my condition management plan to ensure I avoid the dreaded Boom/Bust Cycle. So far, I’ve managed, although my weight training has taken a bit of a back step, sadly.
The difference between me and my phone is if my phone goes flat, I can plug it into power, turn it on and make a call. If my battery goes flat, that is it. Coffee is not going to help. A sugar hit is not going to help. In fact, either might make the situation worse. Imagine if that phone battery could actually go negative and had to be charged back up to zero before use, even when connected to power. THAT is how we can be (not how we can feel, how we can BE) if we are not careful, if we break the rules.
While I was working part-time, I had everything worked out beautifully for me. I got the exercise I needed, the sleep I needed, I did my job well. I never let myself get a flat battery.
While I was not working in the early part of 2020 my plan was to pace up my exercise to build physical resilience in readiness for a new job. With the success of my new treatment, I could do this. There were some interruptions! A knee put me in hospital, then Covid-19 lockdowns followed by a total knee replacement meant things were a bit stop-start, but I was way ahead of where I had been at, say, the end of 2016.
Working full-time has changed how I can arrange my time and also shone a light on the fact the boom/bust cycle is still very much a risk. There have been times at the end of the work day where I quite simply feel my brain shut down. It goes from 90 miles an hour to a dead stop. Nothing I can do about it. The battery is dead. It isn’t just about physical activity, this battery also runs our brain.
It is challenging for people who have no prior experience of these sorts of conditions to understand what happens. After all, many of us, myself included, LOOK fine! It took my daughter some time to come to grips with it, but she now asks “Do you have enough spoons, Mum?” when suggesting something.
I’ve become better at declining social invitations – no, not on an evening before a work day, or no, not two events on one day.
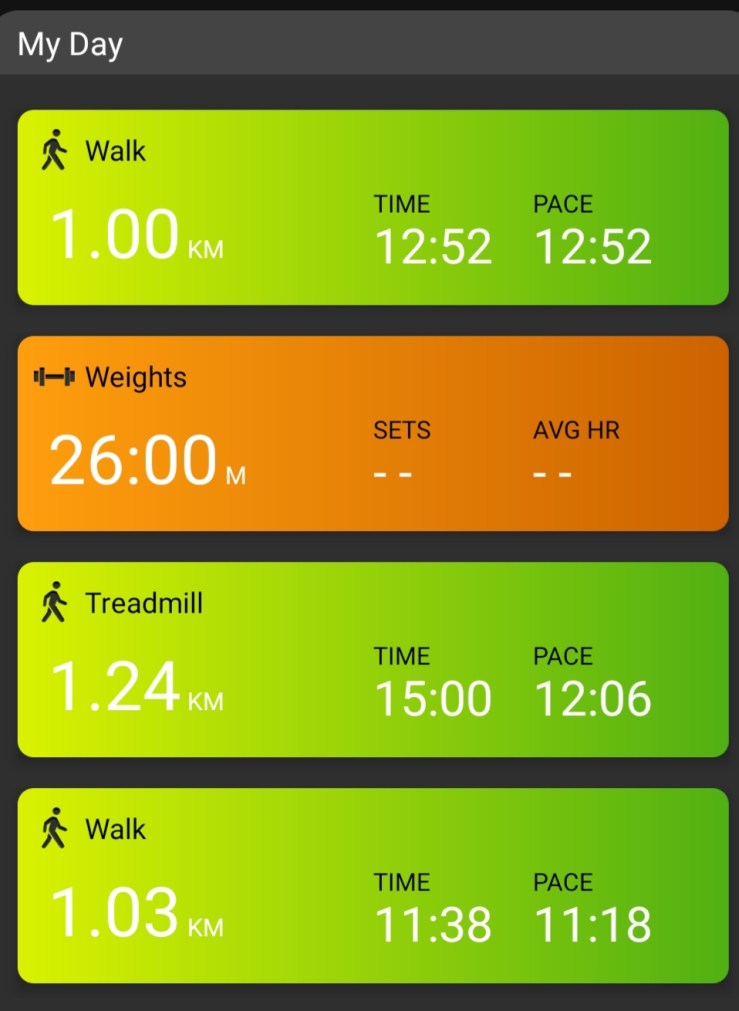
Every activity we do uses battery power. Showering, drying our hair, driving, working, exercising, cooking. In my experience some things use more battery power depending on the time of day: driving is a classic example. Driving for one hour in the morning is not nearly as tiring as driving for one hour in the evening after a day at work. It is almost as if once the battery gets low, it depletes faster. We have to be aware of all these things. I don’t want to cause a fatal car accident because I lose concentration because I haven’t paid heed to my battery level. Look at the pace column of my walks in the image above. the first walk of the day is the fastest, the last is the slowest. This is a constant pattern.
Early in my journey, I would have been unable to do a weight training session and grocery shopping on the same day. That would have used way too much of my battery. Even now, I shower in the evenings. Why? Because I can do it at a slower pace in the evenings and I am not using up vital battery life I need for the work day.
A good night’s sleep should recharge us, you say? We wish that were true. In many cases it is true – unless we have drained too much – then we end up in that negative charge scenario. Not good. However, disrupted sleep is often a symptom experienced by those with chronic conditions. Imagine trying to charge your flat phone, but the charger plug keeps falling out of the phone overnight. In the morning your phone battery is still at only 50%. That can be us.
Strength can fluctuate as well. I happily did 32 kilogram chest press sets one day with every intention of increasing next visit. Next visit I struggled with 25 kilograms. Why? No idea. By no idea, I mean no rational “healthy” explanation. Just that day my body said, “No, not today”.
Endurance is linked to our battery too. Some days I can walk two kilometres easily in one walk – other days I have to stick to three separate one kilometre walks. I’ll feel exactly the same at the start of any walk – then sometimes the body just says, “No, not today”. Part of this is linked to my not having the time available at the moment to consistently Pace UP. Between work and weather I have been limited to grabbing my walks in a somewhat patchy manner which breaks all the rules of pacing. Consistency is key. I’m not getting consistency. I suspect similar applies to the weights.
It is very hard to explain to people what this whole energy thing is like. How we constantly have to be aware of how much battery we’ve used. Healthy people would not, for example, think of having a shower as using energy, or should I say using any great amount of energy. I can assure you, many of the chronic illness community will attest to having to rest after a shower.
In my last article I raved, quite rightly, about the medication I am on. I also stated it hadn’t completely solved the energy/lethargy/fatigue aspect, or the “brain fog”. Despite my writing about energy today, these aspects are still much improved from where I was three years ago. To give some sense of measurement, three years ago I was working 24 hours a week and Saturday morning would always be a recovery morning – I’d do nothing until at least noon. Now I am working 38 or more hours a week and I’m actively doing something by 10 am on Saturdays. I might be at the gym, grocery shopping, doing laundry: I’m active. So a major improvement. And some quantification, which makes me happy!
However, I’ve had to cut my second weight session a week because the energy required to drive to the gym, do weights, drive back and then shower is more than I can manage at the end of a work day. I rarely write any more because usually by the end of the work day my brain has said, “No, not today”. I started this article on December 31, it is now January 16 and I still feel this is very scrappy writing. On the other hand it is a very scrappy topic: as I said I can’t quantify it very well. My thoughts about it come and go: after all, we learn, over time, to live with it. It becomes our new normal. At the same time we recognise that our healthy friends, family and co-workers can be baffled by something they have no experience of and it is not visible.
When I wake up in the morning, assuming I haven’t overdone it the day before, I feel perfectly “normal” just as I did before I became a chronic condition patient. The main difference is at the end of the day I will NOT feel as I did at the end of a day back then. Furthermore, depending how much “charge” I use during the day, I could hit that flat battery state earlier in the day. Other patients will not be as fortunate as I am, I am aware of that. So readers, just because I say I can do something, DO NOT, please do not, assume your mother, father, sibling, friend or co-worker can. They may be “better” or “worse” that I. I am simply n=1 – I’m not a study, I’m just one example trying to explain what it can be like!
As I write, at the beginning of 2021, I am very concerned for the long haul Covid-19 patients, many of whom cite fatigue as an ongoing issue. While the studies of this phenomenon may shed scientific light on ME/CFS, we will also have more chronic patients. My thoughts on society and chronic conditions are expressed in Society and Chronic Health Conditions. As communities, we have challenges ahead.