I last wrote about incidental exercise, but what about a more structured approach to exercise? Many of us with chronic conditions would benefit from exercise. Most of us also probably have doctors in our lives, either general practitioners or specialists (called consultants in some countries) such as a rheumatologist.
Over the Easter weekend an interesting report appeared in the Medical Journal of Australia, “Exercise: an essential evidence-based medicine”. Naturally, I was excited to see exercise receiving coverage in the medical media!
Regular physical activity is highly beneficial for the primary, secondary and tertiary management of many common chronic conditions. There is considerable evidence for the benefits of physical activity for cardiovascular disease, diabetes, obesity, musculoskeletal conditions, some cancers, mental health and dementia. Yet there remains a large evidence–practice gap between physicians’ knowledge of the contribution of physical inactivity to chronic disease and routine effective assessment and prescription of physical activity.
There was a similar report last year out of the UK, “GPs in England ‘unconfident’ discussing physical activity with patients – report”.
Now a nationwide study has revealed that 80% of GPs in England say they are unfamiliar with the national guidelines, and more than one in seven doctors say they are not confident raising the issue of physical activity with their patients.
“Many people have described [physical activity] as the most cost-effective drug we have, yet we are not implementing it properly,” said Justin Varney, co-author of the research from Public Health England (PHE). “This is as appropriate as having a conversation about smoking,” he added.
The medical advice I was given when I became sick was, literally, “Get some exercise.” Not how, what, when, frequency, intensity – just “Get some exercise”. As we know, I did better than that, I went and got an exercise qualification. After that, I asked my rheumatologist what weight he thought it would be safe for me to lift on the leg press, without negatively impacting my condition. His response? “I have confidence in you, you’ll work it out”. Which, in my case given my qualifications and experience, is fair enough. To a patient that is an exercise novice, I know my doctor would not have said that particular phrase. He and I have known each other quite some time now and have a very good patient/doctor relationship. I wouldn’t be writing this article if he had not set me on the exercise path in the first place. I share these conversations to provide real world examples of the above two articles.
Exercise is not a discipline many doctors are trained in, which is fair enough – they can’t be experts in everything and I need my rheumatologist to be an expert in rheumatology! Apart from anything else, a medical specialist would be a very expensive personal trainer. I really do not want to pay his medical charge rate for exercise advice. Look at it this way: a specialist or general practitioner may also send you to a physiotherapist, but do you expect that doctor to BE a physiotherapist? No, you don’t. So we should not expect our doctors to be able to write us a tailored exercise program either.
A member of a chronic illness support group today shared a similar experience, having essentially been told to “figure it out” by one of her doctors.
I recently wrote an article titled “Preventing Tomorrow’s Pain”. I didn’t really write it – I recorded a video. NOW, some time later, when I look back at that video, I can clearly see the improvement in my demeanour/attitude before I walk (after sitting in a conference all day) and while I am walking. Yes, I was pain free the next day and I swam 1,000 metres.
If your doctors don’t mention exercise, raise the topic with them. Really, your doctors don’t need to be exercise trainers, they just need to reassure you and encourage you that exercise will help you manage your conditions. They need to give you a medical clearance to undertake exercise. People like me can do the rest.
The above two articles, from opposite sides of the world, provide clear evidence that just because your doctor may not have mentioned exercise does not mean exercise should be ignored. Exercise may be the best medicine for you, just not mentioned by your doctor. Another contact told me when she offered to do exercise, her doctor was so surprised and said “You’re prepared to do that?” giving my contact the impression maybe he’d just given up over time trying to get patients to exercise. Doctor was very excited, patient exercises and her body does not “turn to concrete”. On a side note, I love that phrase, as it explains so well how many of us can feel if we don’t MOVE!
I use this graphic often: this is what happens if you don’t move. No, you don’t have to be lifting weights, start with simple stretches. Just MOVE it!
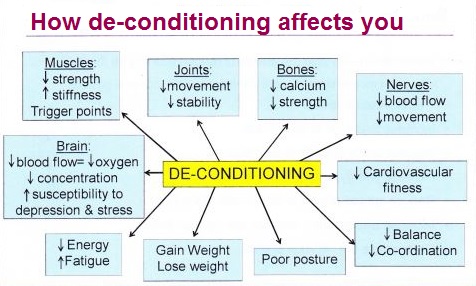
Patients can be reluctant to try exercise as medicine. After all, instinctively we know pain is a warning signal and we believe rest will make it better even though science shows the opposite is true more often than not. We may fear those first few painful steps. A friend said the other day, “the cave you fear to enter holds the treasure you seek”. This, I feel, applies to exercise for so many people. We want the treasure: minimal pain, to be free of opioids, regain functional movement and retain quality of life. The cave is exercise and movement.
You may be reading this because you are searching for a solution. You are researching, perhaps. Do not be afraid to enter the cave. Ask your doctors, raise the topic of exercise with them. If they raise it with you, listen to them. Bear in mind the “how to” of exercise is not their specialty.
If you are ready and willing to try movement as medicine, call me or send me an email.
This article constitutes general advice only and may not be suitable in all situations. You should always seek a medical clearance to undertake exercise if you have medical conditions. Always apply the pain management principles of pacing when starting an exercise program.

[…] our gains and keep building on our achievements. I have discussed exercise in more detail in Doctors and Exercise, so please click that link for a more comprehensive presentation about the importance of […]
LikeLike
[…] Doctors and Exercise – Limberation.com […]
LikeLike
[…] Many noncommunicable diseases are progressive – in other words, the patient may become disabled over time. HOWEVER progression can, in many cases, be slowed dramatically by good management: modern medications, responsible eating, EXERCISE. […]
LikeLike
[…] a great note, for PsA management, J had certainly been moving. Movement is Medicine! However, J had probably used up more spoons or internal battery than she had available. All that […]
LikeLike
[…] I find, are often (not always) good at telling patients to get exercise, but that is where the advice stops! How is left up to the […]
LikeLike