My apologies for my silence over the last six weeks or so. I counted my chickens before they hatched.
On March 12 I published Changing Medications – What Can You Expect?. At that point it was roughly ten weeks since I had changed my medication for psoriatic arthritis (PsA) and I was finally feeling as if the new medication was starting to kick in. I was a little overly optimistic, as it turns out.
Also, although not mentioned in that article, the whole situation became more complicated when I slipped/tripped and fell in the shopping centre car park on March 8. What I initially thought was a simple trip ended up with me back in my orthopaedic surgeon’s office. To cut a long story short, it was decided the time had come to replace my right knee. If you are new to my story, I had the left knee replaced in 2020.
The problem was the slight improvement I’d got overly hopeful about in March did not continue. I was quite quickly back to waking in considerable pain and struggling with malaise and energy levels.
At the time I saw my perioperative physician I was still on 400 mg of Celebrex and 15 mg of Prednisolone a day. In order to undergo surgery on May 10 (the scheduled date) I needed to reduce the Celebrex to zero by May 1 and the Prednisolone to 2.5 mg per day by a week before the surgery. Was this going to be a challenge, I wondered to myself. I certainly didn’t want to just stop the Celebrex cold turkey on May 1 as clearly I was still in need of it to function on a daily basis. I’d needed friends to drive me to a myotherapy appointment and my pre-op Visionaire scans. Essentially, I wasn’t too chipper.
I discovered I had another infected tooth – maybe THAT was the problem? Had that tooth removed. It was a rather complicated event as the tooth was part of a double crown. I spent over an hour in the dentist’s chair, most of that time was spent removing the crown and temporarily recrowning the uninfected tooth. The actual extraction was a minor part of the visit. However, removing the tooth did nothing to improve my overall inflammation.
On April 17 I could see May 1 looming and decided I’d see if reducing the Celebrex was at all possible. Celebrex comes in capsule form – you either take a capsule or you don’t, there’s no pill splitting here! So I dropped from 400 mg to 200 mg on that Monday. Deliberate timing, as I had a GP appointment on the Tuesday. If anything went wrong, I already had an appointment! I also had accepted another kind offer from a friend to drive me to that appointment.
I woke up on the Tuesday in a very unwell state. While I managed to sit up in bed and get my feet to the floor, I could not actually stand up. This was a bit of a worry, to say the least. As gross as this sounds, I’m sharing for transparency: I was very worried about actually getting to the toilet in time. I tried using my walking stick to give myself some leverage, but doing so hurt both my hands and my shoulders due to the angle. Eventually I managed to stand upright and shuffle to the bathroom. While I was on my feet, I shuffled to the front door and unlocked it from the inside – if I had to call an ambulance, at least they could get in. Obviously I was in no position to start reducing my anti-inflammatories!
After various communications between my GP, rheumatologist and knee surgeon, the knee surgery was cancelled for the time being. My CRP and ESR inflammatory markers were rather high and THAT was while I was on all this medication. What would those markers have been reading if I was on no anti-inflammatories?
I did a damn good job on my rehab of my first knee and it is FANTASTIC! I want to be able to achieve the same result with the second knee replacement. At that point in April I was able to walk a mere 800 metres at a time because my ankles were so painful, the left one in particular. I knew that the extra loading of that ankle while recovering from surgery for the right knee could be very problematic. All things considered, cancelling the May 10 date was sensible, but very disappointing. I want the knee done, but there is no point in being a less that optimal patient if that can be avoided.
My next new medication injection was May 4 and I was getting closer to the 24 week mark – SURELY it would start working!
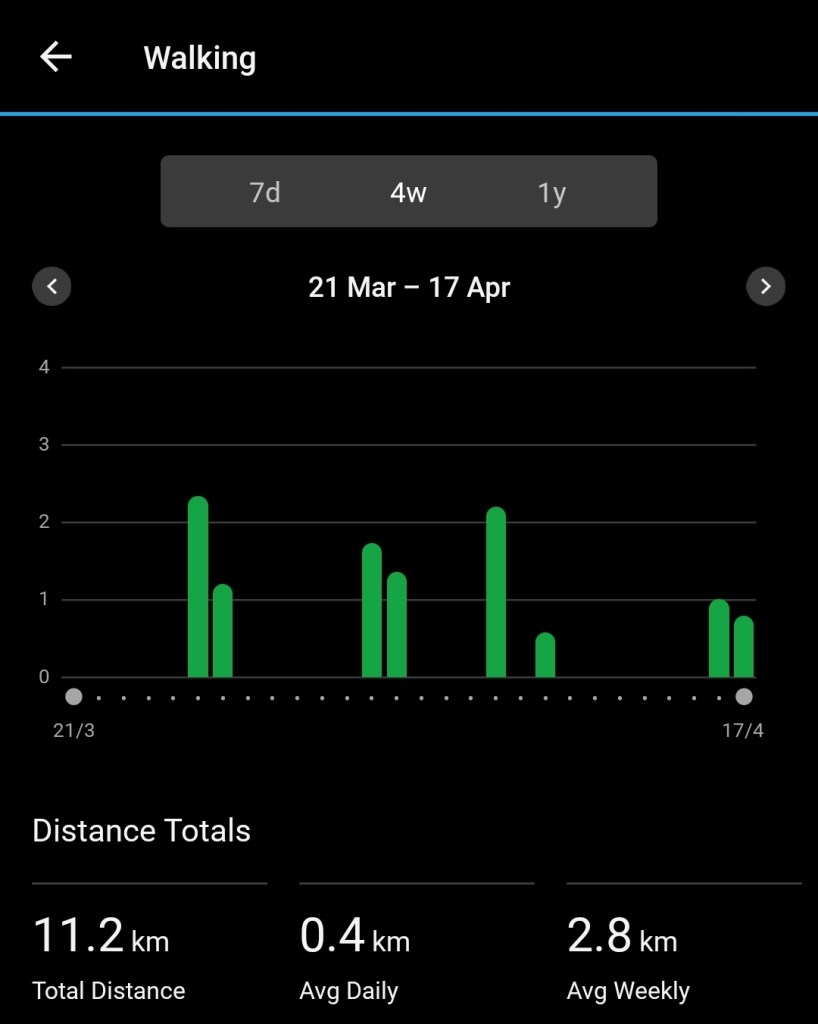
On May 4 (a Thursday) I gave myself the scheduled injection. Nothing much changed until Monday May 8. I did feel an improvement. I managed to walk 1.5 km in one walk. In total I walked 3 km for the day. I have slowly built up during the week and on Friday I walked a total of 4 km over three walks – I’d hit my old goal of 4 km for the day. Saturday I walked 2 km twice. The possibility of post-op rehab is now looking more achievable! I’ve even walked at my favourite walking spot, shown in the picture above.
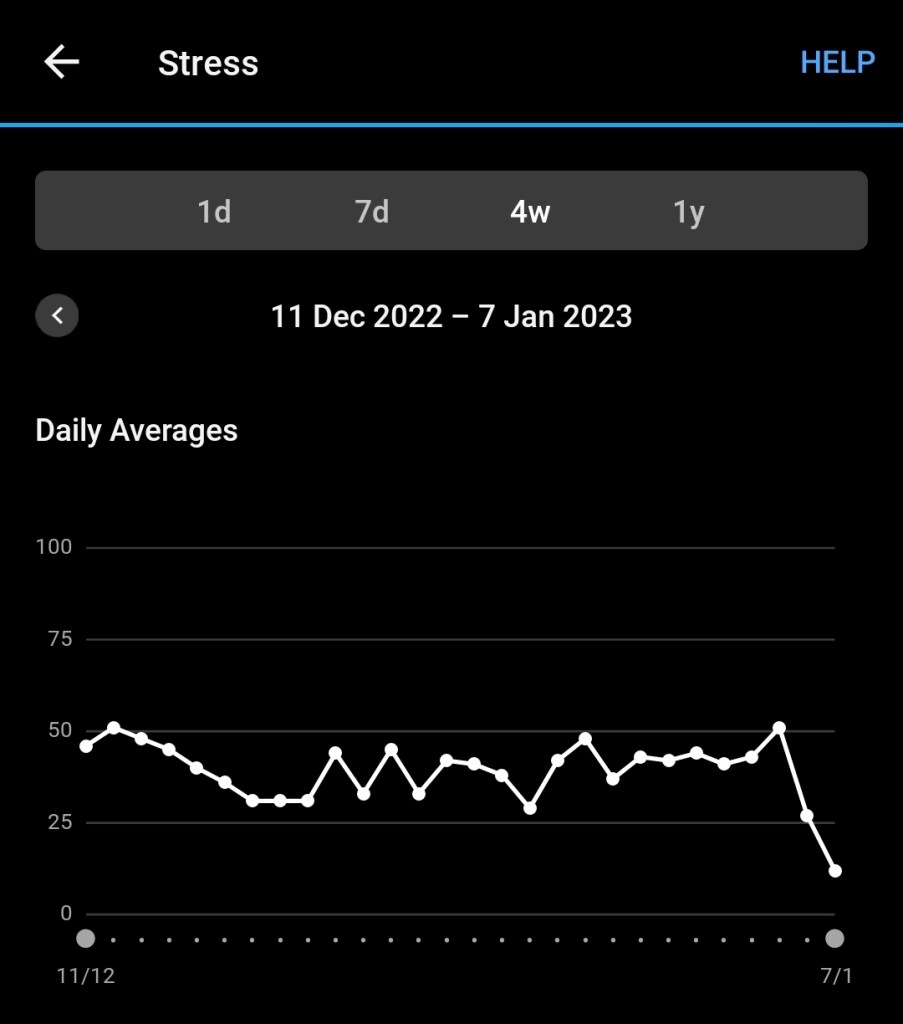
For those into graphic representation, here are the last 8 weeks. PLEASE NOTE Garmin changes the scale between the two periods, which makes the March/April bars look WAY higher than most of the April/May bars. And of course I haven’t finished today! Look at the total kilometres: 11.2 km versus 58.9 km

HOWEVER – I’m still on those same dosages of anti-inflammatories. I asked the GP about a possible test reduction and she was rather adamant that I give myself two weeks before we try to change anything. I haven’t even mentioned the pain medication I’m also taking or the Voltaren gel I am using on my hands and ankles.
While all this was happening, my rheumatologist scanned me for gout. The CT scan came back negative, which as the rheumatologist said is both a good and a bad thing. While it is good I don’t have gout, we are back to square one. Why is my inflammation so high? Is it merely that the new medication is taking its own sweet time to be effective? Or is my body being difficult?
Speaking of difficult bodies, I also did something rather adventurous. Click the image to go to the website.
While I am not going to go into detail about this test, it has been useful to me. My report was 29 pages long. To give you an indication, this is a summary of my genotype for the genes the test currently looks at.

We have changed two of my medications as a result. We also know to watch out for certain other medications in the future. This test does not yet cover every medication known to science, but it covers a lot. If you are interested, I suggest you speak to your GP about whether it may be useful in your situation. Yes, it is rather costly on a limited income but I see it as an investment in my health, given my situation.
Right now I am nervous that I am again counting my chickens before they hatch. Today is day eight of incremental improvement. I’ve managed to walk 4 km three days in a row, hopefully today as well. I have more energy. I’m writing. I haven’t ventured back to the gym yet, although I desperately want to.
In summary, as I said in my first article on the subject of changing medications, it is often not as simple as opening a different pill bottle. Even as I write, I do not yet know if this medication is going to be effective for me, but at least I have had eight straight days of improvement. I can exercise reasonably well again. This morning I woke with far less pain in my hands! So I’m crossing my fingers. The last blood test results showed a slight improvement in my inflammatory markers.
If you or someone in your life is changing medications, please be gentle. Be understanding. Be aware it may NOT be smooth sailing.