There are patients whose conditions have progressed in ways many of us cannot imagine, despite their best efforts and the efforts of their medical teams. One such patient is Sam Moss. In 2010 Sam was diagnosed with rheumatoid arthritis, but that was just the start of her medical journey: she has since been diagnosed with other conditions.
12 months after my leg broke, my right femur was also showing signs of disease on MRI with bone marrow involvement so a rod had to be placed in that to prevent an imminent break and repeat medical emergency like we had with my femur break in 2014. I am constantly dealing with multiple foot fractures and none of my broken bones in my legs or feet will heal.
Source: My Medical Musings
Sam now runs a support group for those facing medical challenges, Medical Musings With Friends. It is a closed group, very supportive. If you would like to join, click the link. Membership of the group is also a rapid introduction to how severely some conditions can progress, even with the best medical care and patient tenacity in the world.
My objective, for myself and my clients, is to slow condition progression and manage pain where possible. Yes, sometimes our medical conditions do take control as described above, but many of us, in collaboration with our medical teams, can control our conditions, be the master of our medical destiny. We, as patients, want to ensure we don’t give those medical conditions any head start if we can help it. If, like me, you are lucky enough to have a choice, don’t waste that opportunity – there are many out there who would be very grateful to be in our situation. Chronic condition severity is a spectrum and we are all somewhere along that spectrum trying to do the best we can.
I support the recent rescheduling of codeine. I definitely think the change over could have been better planned, as it seems many where left without codeine OR any alternative. Those who ensured they had prescriptions found there was no stock available in pharmacies.
In the past I have used Panadeine Forte after having teeth extracted. I’ve used Tramadol (another opioid) about three times a year. I’m not against codeine per se, it has a place in medicine. Taken under medical supervision when appropriate it is a useful drug. Self-medicating with over-the-counter supplies regularly can lead to problems.
There is a reason why morphine and its equivalents feature on the World Health Organization (WHO) list of essential medicines, along with oxygen, steroids and penicillin. These are virtually irreplaceable in certain situations, including severe burns, postoperative recovery, cancer pain and palliative care. But there is no additional benefit of opioids over simple drugs like paracetamol and ibuprofen when taken for toothache, back pain, migraines, asymptomatic kidney stones, muscle sprain, fractures and many other conditions associated with chronic pain. Here, opioids are not just unhelpful but they can also worsen pain, apart from the fact that they are addictive and fatal. Therefore, it’s best to avoid them for all but a narrow range of conditions that you should discuss at length with your doctor.
Source: Ranjana Srivastava, The Guardian
Early in my journey, one of my problems was I was VERY stiff and sore when I got out of bed in the morning. I had two choices, A) try a pain killer of some sort or B) move. Back then I really had no idea what I was doing, I was on a learning curve. I found very quickly if I walked, even as little as a few dozen steps, the pain and stiffness subsided. Clearly, for me at least, moving worked.
Now, some years later and professionally trained, I am much better at linking my discomfort levels to what I have, or have not, been doing. This last week has been a classic. For whatever reason I had several days when by six o’clock at night I was out of energy. I mean totally out of energy. I’d arrive home from work and flop on the couch and be unable to move. Which, for me (and many others) is a very bad plan. The stiffness and pain returns. Just getting up of the couch, I was stiff and had to straighten my back. Not how I like to be. As anyone with chronic conditions knows, sometimes there are no obvious reasons for “flares” they just arrive unannounced. I had my thyroid function and iron levels checked, they were fine. I had again had a change to my routine, which my conditions do not seem to like very much, so that may have been the trigger. While understanding why is helpful to prevent future flares, I haven’t managed to detect a pattern (flares are rare for me), I just needed to get back on the horse.

When I ensure I move enough and keep my strength up I am pain free and have very little, if any, stiffness. A little discomfort every now and then if my lumbar spine reminds me “Hey, I’m here, don’t forget I’m here”. I reassure my facet joints I haven’t forgotten them, do some stretches and core strength work and they settle down.
Best-practice recommendations now are focused on self-management and self-support: moving away from opioids, prescription or otherwise, and focusing more on allied healthcare and other non-drug methods to minimise pain. Pain Australia has launched a campaign called RealRelief to help people move beyond codeine and take control of their pain. Their foundational idea is that most people with chronic pain can improve their lives without opioids or surgery as long as they are appropriately supported to do it.
The caveat there is the support. Hard to move beyond pain when you are by yourself and suffering.
Source: Making codeine prescription-only was right. Where do we go from here? – The Guardian
No, I do not take painkillers in these situations. I have an edge, of course: I did the PACT program. I know and understand the science behind the recommendations. I recognise it can be difficult for someone without that knowledge and support to resist reaching for the pill packet, which MAY give them some relief in about twenty minutes. I can walk 500 steps and be pain free a lot faster than the twenty minutes it takes the pills to work, without the associated health risks of codeine. I also stress the MAY (give relief). Anyone with chronic pain will attest to the fact sometimes the pain meds just do not even touch the sides.
What if I took Option A and reached for the pain killers instead of moving? What would happen? I’d get worse, that is what would happen. That is the cold, hard truth of it.
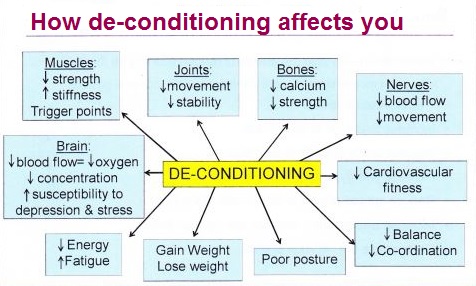 If I reached for the painkillers, I’d then have a foggy head, so I’d lie (or maybe sit) down. I’d be doing nothing to actually strengthen or stretch my muscles or counter any of the negative affects shown above. I would progressively deteriorate over time and be on a downward spiral. Then my quality of life would suffer. Josh, another chronic condition patient, has written a very amusing story about having a couple of beers. Now, Josh is one of those patients I referred to in my opening paragraphs, he has done everything possible yet because of his medical situation he is on some pretty strong stuff. I may ultimately end up in a similar situation, but I’m going to do everything in my power to delay such a situation. I also do NOT see getting worse as inevitable for me. I like being able to have a nice wine or two over dinner or with co-workers on a Friday night without sounding smashed (to quote Josh’s wife).
If I reached for the painkillers, I’d then have a foggy head, so I’d lie (or maybe sit) down. I’d be doing nothing to actually strengthen or stretch my muscles or counter any of the negative affects shown above. I would progressively deteriorate over time and be on a downward spiral. Then my quality of life would suffer. Josh, another chronic condition patient, has written a very amusing story about having a couple of beers. Now, Josh is one of those patients I referred to in my opening paragraphs, he has done everything possible yet because of his medical situation he is on some pretty strong stuff. I may ultimately end up in a similar situation, but I’m going to do everything in my power to delay such a situation. I also do NOT see getting worse as inevitable for me. I like being able to have a nice wine or two over dinner or with co-workers on a Friday night without sounding smashed (to quote Josh’s wife).
I like driving, dining out, dancing and swimming. I want to keep my body as functional as possible for as long as possible. Don’t you?

Once we start on that downward spiral, we find we have so many restrictions. Such restrictions may include:
- Limited driving ability (no drugged driving, for example)
- No alcohol
- Progressive physical deterioration due to inactivity
- Loss of social interaction
- Reduced working hours or incapacity to work
- Depression and/or anxiety
No, it is NOT easy to start the movement momentum. Sometimes it is not easy to keep it going. Yes, it does require willpower and resilience. Yes, it requires mental strength to take those first steps in the morning or after sitting for too long.
Yes, as a community we need more support. Refer again to the above article: “as long as they are appropriately supported to do it“. I was lucky enough to be accepted into the PACT program but there are not enough of those programs available yet and there are waiting lists.
Think about where you want to be in five years time. Do you want to have a body that can support the quality of life you desire or do you want to be staring down that spiral?
Talk to your doctors, ask them if movement as medicine is an option for you.
“It’s [resilience] vital to the process,” he explains. “I’ve seen patients who, under the circumstances, might want to just give up, but they don’t. In fact, they thrive. Their resilience helps them cope and keep moving forward to find a solution. They say, ‘I’m going to make it no matter what.’”
…
“We used to put patients on bed rest for pain. Not anymore,” says Dr. Tom. “Staying physically active is critical for pain management, as it releases endorphins which can improve your mood and even ease pain.” People who don’t move can get tight muscles, joint pain, muscle strain and spasms, which can worsen existing pain.
If you’d like to give moving a try, click on Contact and send me an email.


Published by