What comes first? The chicken or the egg?
PLEASE NOTE: There is MUCH more to the question of pain than I cover is this very short video. Here I am looking at ONE small incident to highlight how it can be contentious, even with relatively small (wrist) body parts (which may be being disproportionately painful).
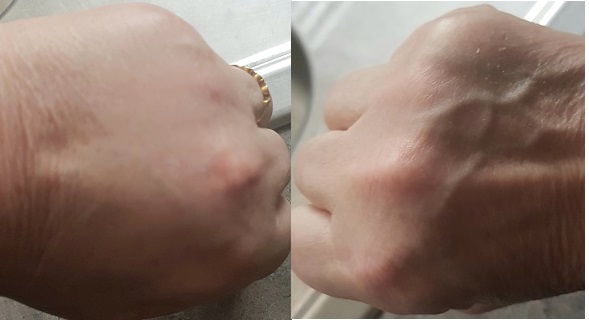
In the above video I compared my wrist pain to my post-op total knee replacement pain. Please hear that in context: with the knee I was in hospital, a myriad of medical staff ensuring the pain was WELL MANAGED. The net result is yes, the wrist was worse.
I’m using video a bit at the moment to protect my wrist as it heals. I’m new at this video game, so please bear with me!
I wrote in a bit more detail about my current health challenges at Movement As Medicine for anyone catching up: the wrist in question was already showing signs of being something different to the rest at that time.