I mention having psoriatic arthritis (PsA), yet I’ve never explained in layman’s terms what it actually is. This is partly because initially I was diagnosed with rheumatoid arthritis (RA). There is reasonable general knowledge about RA so I didn’t write about it specifically at the time. There are over 100 forms of arthritis – PsA is just one.
PsA is also not to be confused with PSA. PSA stands for Prostrate-Specific Antigen. Usually in reference to the PSA test. In text the difference is clear, but I have had some funny looks from people when I’ve spoken PsA. Even in writing, for example on Twitter, people get confused thinking I’ve just made a typo with the little “s”, but I’m a woman, so….. how could PSA apply to me? It doesn’t. PsA does.
PsA is not nearly as well known as RA is. I know a fellow patient who just tells people she has RA rather than have to repeatedly explain what PsA is. All the PsA patients I know have run into healthcare workers who’ve never heard of it. It is quite similar in some respects to RA, but there are some major differences.
As the name implies, it is related to the skin condition psoriasis. PsA was officially recognized as a distinct disease in 1964 by the (now) American College of Rheumatology. The prevalence in the general population is estimated at around 1%, however the estimates vary. I’ve cited 1% as it is the figure I see most often. PsA is not technically a rare disease. While definitions of rare diseases are different in different jurisdictions, most definitions are around a prevalence in the population of 0.05%. Even so, at 1% we are not the most common patients around either!
Up to 30% of people with the skin condition psoriasis may develop PsA. I’ve seen numbers as high as 42% given in some studies, but for general understanding, 30% will suffice.
For readers who have never seen psoriasis there are different types and they look different. Here is my ankle during one recent flare as an example.

The genetics of PsA are still being investigated, but strong genetic links have been found. It tends, therefore, to run in families. My doctors and I suspect I am third generation.
PsA is classified as a spondyloarthropathy. It is an IMID – immune mediated inflammatory disease. There are five different types of PsA and a person may have more than one type:
- Symmetric arthritis
- Asymmetric arthritis
- Distal interphalangeal (DIP) predominant
- Spondylitis
- Arthritis mutilans
PsA can affect just about any joint in the body, it is not fussy (RA is a little more choosy). It moves around the body. It loves (in my case) entheses – of which we have more than 100! Entheses are where a ligament or tendon inserts into the bone. It can be very “ouchy”. It is also a disease that affects men and women equally.
Getting a formal diagnosis can still prove difficult. I’m a classic example as I was originally diagnosed with RA. I did not have really visible psoriasis at the time. My psoriasis blew up while I was on hydroxychloroquine – this was the driver of my new diagnosis. Hydroxychloroquine has been shown to exacerbate or induce psoriasis. PsA will also express itself in some patients before the skin condition presents itself. There are no easy tests to diagnose PsA, it is often a process of elimination of other possibilities. I was fortunate to be diagnosed and therefore treated early in my journey. We slowed the progression of the disease before too much damage was done.
Comorbidities are common:
Epidemiological studies have shown that patients with psoriatic arthritis (PsA) are often affected by numerous comorbidities that carry significant morbidity and mortality. Reported comorbidities include diabetes mellitus, obesity, metabolic syndrome, cardiovascular diseases, osteoporosis, inflammatory bowel disease, autoimmune eye disease, non-alcoholic fatty liver disease, depression, and fibromyalgia. All health care providers for patients with PsA should recognize and monitor those comorbidities, as well as understand their effect on patient management to ensure an optimal clinical outcome.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5298365/
I’ve had cysts develop that in one case was dissecting a leg muscle, in another case the cyst drilled a “huge” (that’s a quote from the surgeon) hole in a toe bone and I needed a bone graft. This sort of thing won’t happen to every patient, of course, but is an illustration of the sorts of challenges patients face. Nodules can grow on tendons – I have a few of those. Cognitive impairment, otherwise known as “brain fog” is common. Fingers and toes can swell to look like sausages, this is called dactylitis. I’ve had a whole hand swell up, while the other remained fine. Here is a comparison of my hands at the time.
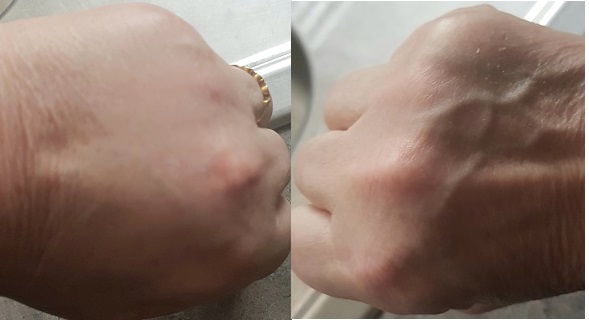
I’m slowly losing fine motor control of my fingers. It is annoying, but manageable so far.
Malaise is another symptom that I don’t experience often, but it does pop up from time to time. Just feeling crappy, basically. Feeling very blah! Like pain flares, malaise can come and go unpredictably.
Fatigue or lethargy is a symptom that doesn’t get nearly enough attention. It can be debilitating and impact on the patient’s ability to manage the condition appropriately. Exercise is considered critical in the management of PsA, but if the patient has no energy, nothing in the tank, exercise can be challenging. This improves with exercise, over time, but it does take dedication on the part of the patient. Eating and sleeping properly go without saying, naturally!
Flares can appear out of nowhere and disappear as quickly as they arrived. I recall once waking with an excruciatingly painful wrist. Eight hours later it was 100% normal. Flares may also linger. I’ve had steroid shots in both shoulders, vastly different to my painful wrist experience. PsA is notoriously unpredictable. It can destroy your finger and toe nails. Anyone who follows me knows, for me that would be a devastating event! Hence the feature photo of my pride & joy!
No, I haven’t specifically mentioned pain, have I? Everyone’s pain is different. For the most part (aside from the occasional flare or when a medication stops working) I am pain free. That’s due to a combination of factors: early diagnosis therefore early treatment, exercise, appropriate medication. When my previous medication stopped working, I was in heaps of pain. I detailed that in “I Sat in my Car and Cried“.
This is not in any way a medical article, it is a short summary of what PsA is and can be for the newly diagnosed and family and friends. Below I have listed authoritative links readers may find relevant. I will update this list from time to time as new articles become available. Whatever I publish today will likely be out of date tomorrow as PsA is a condition that medical science is still investigating and learning about. The photos I have used are my own.
Informative Links:
Psoriatic arthritis – new perspectives (National Library of Medicine, PubMed) Very informative! (added here 09/05/2023)
Psoriatic arthritis: epidemiology, clinical features, course, and outcome (BMJ)
The Genetics of Psoriasis and Psoriatic Arthritis (The Journal of Rheumatology)
Genetics of psoriatic arthritis (PubMed)
Types of psoriatic arthritis (Psoriatic Arthritis Info, sponsored by AbbVie)
Spondyloarthropathies (HealthLinkBC)
Enthesitis and PsA (Arthritis Foundation)
Psoriatic arthritis – diagnosis (Mayo Clinic)
Understanding Arthritis (Arthritis Australia)
We Don’t All Look Sick: Invisible Illness (Limberation)
We Need Mental Health as well as Physical Health (Limberation)